The state of wound care in SA
In this comprehensive interview, we spoke to wound expert Dr Ethel Andrews to get the low-down on South African best practices for wound care.
Dr Ethel Andrews
Dr Ethel Andrews

Medical Academic (MA): Hi Dr Andrews, could you clarify the current state of wound care guidelines in South Africa and how practitioners navigate clinical decision-making?
Dr Ethel Andrews (EA): Firstly, I think it’s crucial to address a common misconception from the outset. When people ask about South African wound care guidelines, they often assume we have comprehensive national protocols. The reality is quite different. There are no specific, comprehensive wound care guidelines in South Africa, except for certain topics covered by the Wound Healing Association of South Africa, such as negative pressure wound therapy guidelines. However, these don’t constitute a complete set of guidelines that inform practice across the country.
What we do instead, and what makes considerable sense, is adopt international guidelines. If the entire global medical community is following evidence-based practices, we align ourselves with these standards and adapt them to our local circumstances. The onus lies on South African clinicians to refer to international guidelines, which represent the standard that the rest of the world follows.
MA: Could you elaborate on which international frameworks you particularly rely upon for wound assessment?
EA: I’ve aligned my practice with the wound bed preparation and TIME paradigm, which is essentially a living document that evolves regularly. The most recent iteration was released in 2024 by Sibbald and colleagues, and it’s what most wound care professionals worldwide reference.
This paradigm has undergone significant evolution since its inception. When it was first introduced in 2000, it focused exclusively on chronic wounds and primarily addressed local wound management - essentially how to assess the wound itself, what to do with tissue, and immediate wound care decisions. However, the 2024 version represents a fundamental shift towards holistic patient care.
The current paradigm emphasises that you must begin by identifying the underlying cause of the wound. If you’re treating a diabetic patient with a foot wound, you’re dealing with a diabetic foot ulcer. If the patient has circulatory problems, that becomes a critical factor in your treatment approach. You simply cannot ignore the broader health context when developing a wound management strategy.
MA: You mention holistic patient evaluation. Could you explain why this approach has become so central to modern wound care?
EA: The shift towards holistic evaluation represents a fundamental change in the clinician-patient relationship and our understanding of healing processes. Previously, wound care operated on a paternalistic model where I, as the clinician, would make all decisions and simply inform the patient of the treatment plan. We’ve moved away from this approach because we recognise that patients have their own values, concerns, and life circumstances that directly impact healing outcomes.
The new paradigm addresses what we call patient and family-centred concerns as the second pillar of assessment. In my practice, I encounter these concerns daily. A patient with a surgical site infection might worry about travel costs for frequent appointments. A mother of a child with burn injuries will ask about potential deformities or scarring. A diabetic patient facing potential gangrene is naturally concerned about amputation. These aren’t peripheral concerns - they’re central to the healing process.
We’ve discovered that patient anxiety actually delays wound healing. You cannot treat a wound in isolation whilst ignoring what’s troubling the patient psychologically and practically. This realisation has revolutionised how we approach wound care.
MA: This leads to an important clinical question about wound healing potential. How do you determine whether a wound is actually healable?
EA: This is the third critical factor in the contemporary wound bed preparation paradigm. Despite our best intentions and interventions, not all wounds possess the ability to heal. We must categorise wounds into three types: healable wounds, maintenance wounds where we’re preventing further complications, and completely unhealable wounds.
Consider a patient with a venous leg ulcer who requires compression therapy. If this patient consistently removes their compression bandages upon leaving the clinic, they become non-compliant with essential treatment. Despite the best clinical intentions, financial investment, and therapeutic efforts, non-compliance renders the wound either non-healable or suitable only for maintenance care. This classification is crucial for setting realistic expectations and allocating resources appropriately.

We’ve discovered that patient anxiety actually delays wound healing. You cannot treat a wound in isolation whilst ignoring what’s troubling the patient psychologically and practically.
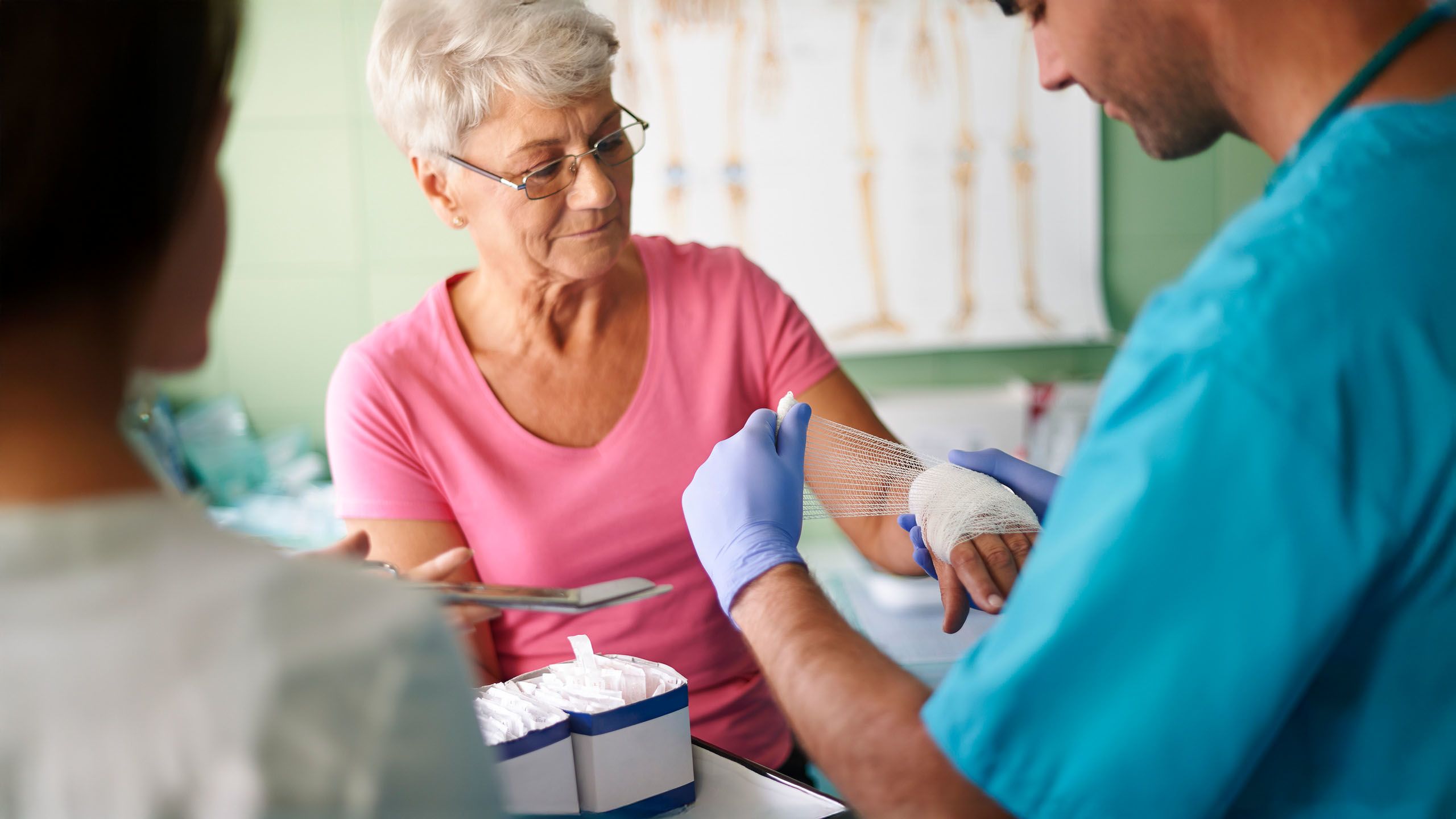
MA: What are the essential steps for cleaning and debriding wounds in the South African context?
EA: Cleansing and debridement are absolutely non-negotiable components of wound care - you cannot omit these steps. However, I’m concerned that some practitioners still apply traditional approaches, simply removing old dressings and applying new ones without proper cleansing or debridement.
The rationale for thorough cleansing includes reducing bioburden, enabling accurate wound assessment, removing debris and previous dressing materials, controlling odour, and creating an optimal healing environment. In terms of debridement, we must remember that wounds cannot heal in the presence of non-viable tissue.
As a nurse, I’m qualified to perform autolytic debridement using water-based ointments that allow the body to naturally debride itself, or enzymatic debridement using dressings with active ingredients that selectively distinguish between viable and non-viable tissue. Sharp debridement is another option, but certain cases, particularly full-thickness burns, require surgical debridement and immediate referral. The key skill lies in recognising when conservative debridement is insufficient and surgical intervention becomes necessary.
MA: How do you differentiate between infected and colonised wounds, and what are the treatment implications?
EA: This question addresses one of the most complex aspects of wound care because wounds exist on a spectrum. They progress from contaminated to colonised, then critically colonised, infected, and finally to systemic or spreading infection. We follow international consensus guidelines from 2022 for this assessment.
Contaminated wounds require no intervention because the patient’s immune system can manage the bacterial load. Colonised wounds contain multiplying bacteria, but the host retains the ability to overcome them and heal naturally. Treatment becomes necessary when wounds reach the infected stage, where we apply topical antimicrobial dressings to reduce bioburden whilst simultaneously addressing underlying factors like diabetes management or autoimmune conditions.
Systemic antibiotics are reserved exclusively for patients who are systemically unwell - those presenting with fever, elevated white cell counts, or increased infection markers. This approach aligns with antibiotic stewardship principles. If we prescribed antibiotics for every skin break, we would accelerate the development of multi-drug resistant organisms. When patients truly need antibiotics, they would prove ineffective due to resistance from overexposure.
MA: What principles guide your selection of wound dressings, particularly regarding moist wound healing?
EA: First, we must understand that moist wound healing has been evidence-based practice since Winter’s research in the 1960s. Yet remarkably, even in 2024, some practitioners still advocate leaving wounds open to dry. This approach is fundamentally incorrect.
Desiccated wounds prevent epithelial cell migration across the wound bed, cause unnecessary pain, delay healing, and in the case of weeping wounds, increase costs through frequent linen changes and additional nursing time. The principle is straightforward: dry wounds require moisture-donating dressings like occlusive products, whilst wet wounds need absorbent dressings.
Dressing selection depends entirely on exudate levels. Options include foams for moderate exudate, alginates for higher absorption, or negative pressure wound therapy for heavily exuding wounds. There’s no universal “first-line” dressing - your choice must match what the wound presents. If you remove a dressing and find minimal exudate, your current dressing may be inappropriate. If the dressing is saturated, you need greater absorption capacity.
MA: When do you recommend systemic antibiotic therapy, and how do you navigate the challenge of multi-drug resistant organisms?
EA: Systemic antibiotics are indicated only when patients are systemically unwell - presenting with pyrexia, elevated white cell counts, or increased infection markers on blood tests. This targeted approach is essential given our current crisis with multi-drug resistant organisms.
South African hospitals are grappling with carbapenem-resistant Enterobacteriaceae, Klebsiella, Clostridium, and numerous other resistant organisms emerging from community settings. If we continue inappropriate antibiotic prescribing, we accelerate resistance development. We’re approaching the limits of available antibiotics, so preservation of effectiveness is crucial.
Even for burns, we don’t routinely prescribe prophylactic antibiotics unless dealing with specific surgical site infection protocols. General wound care - abrasions, pressure injuries, or routine wounds - should not receive systemic antibiotics without systemic indication.

In terms of debridement, we must remember that wounds cannot heal in the presence of non-viable tissue.
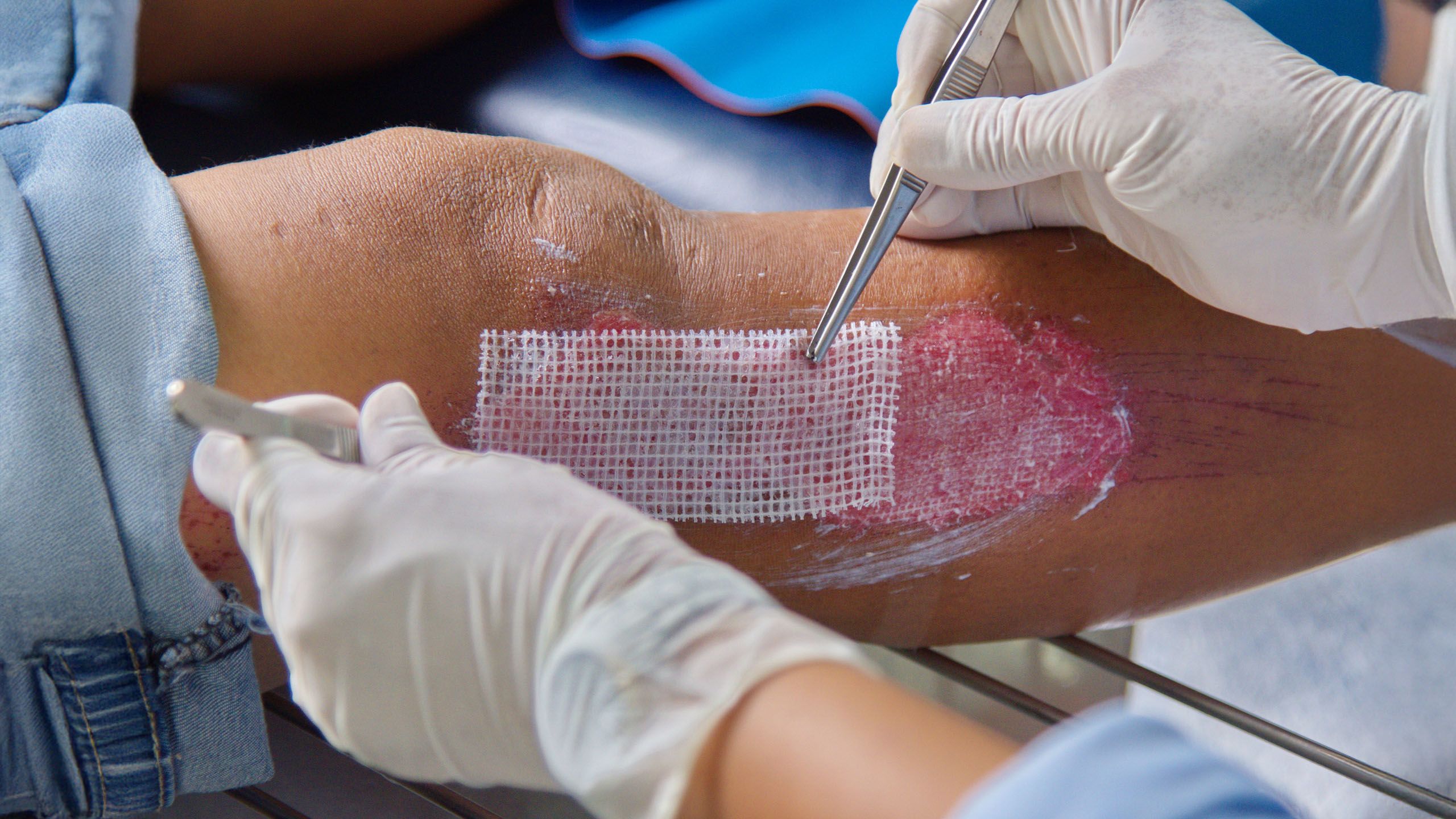
MA: Diabetic foot ulcers represent a significant challenge. How should healthcare workers approach this complex condition?
EA: Diabetic foot management exemplifies why modern wound care requires multidisciplinary approaches. Here’s a sobering statistic: many patients admitted with non-healing foot wounds are unaware they have diabetes. They seek treatment for a wound, and diabetes is diagnosed during hospitalisation through blood glucose or HbA1c testing.
Effective management requires multiple specialists. Diabetic educators explain disease progression and neuropathy prevention. Physicians manage glycaemic control, targeting HbA1c levels below eight or nine. Dietitians address nutritional needs, including high-protein diets and micronutrients like zinc and vitamin C essential for wound healing.
Foot structure changes necessitate orthotist or podiatrist involvement for hammer toes, rocker-bottom feet, and other deformities. Wound specialists manage the actual ulcer. Orthopaedic surgeons address fractures that patients may not feel due to neuropathy. Vascular surgeons handle circulatory complications that frequently accompany diabetes.
The complexity is immense because diabetic foot patients present multiple interconnected challenges requiring specialist expertise. Prevention remains paramount - education at diabetes diagnosis about pressure injury prevention is infinitely better than treating established complications.
MA: Finally, what are your recommendations for pressure injury prevention in resource-limited environments?
EA: The foundation of pressure injury prevention is observation and assessment. Patients can develop pressure injuries within two hours on casualty stretchers, so assessment must begin immediately upon entry to any clinical setting.
Risk factors include perspiration, extreme weight variations, advanced age, and decreased responsiveness. Visual skin assessment is crucial because patients often arrive from care facilities or home environments with existing damage - perhaps a blister on the heel or sacrum representing stage one pressure injury.
Various risk assessment scales exist, but the fundamental principle is simply observing your patient. Look at their skin, assess their presentation, and recognise that non-responsive patients are automatically high-risk candidates. In resource-limited settings, this observational approach requires no expensive equipment - just clinical awareness and systematic assessment.
I hope all this clarifies that, while we don’t have specific South African wound care guidelines, we maintain high standards by adapting international evidence to our local context and resource constraints.
Dr Ethel Andrews is an Advanced Wound Specialist who holds a Doctorate in Burns from the University of Witwatersrand. She is the first African recipient of the Baskent University Nursing award for her contribution to the advancement of nursing.
To view a CPD-accredited recording of a wound care webinar presented by Sr Liezl Naude, click here: http://bit.ly/45Icq6q.
Please notify John.Woodford@newmedia.co.za once you have watched the recording, with your name, surname and professional registration number.